Prepare For Defective Herd Immunity: It’s Coming – OpEd
As advanced economies have failed to contain COVID-19, fattened epidemic curves could make the global pandemic longer and deadlier.
In my new report, The Tragedy of Missed Opportunities, I have examined the huge human costs and economic damage of COVID-19 [for the report, click https://www.differencegroup.net/coronavirus-briefs ].
Before advanced economies began to flatten the epidemic curve, they fattened it for 6-8 weeks. This could prolong the global pandemic and cause secondary waves of imported infections and new virus clusters worldwide.
Defective herd immunity
Like the United States, most of Europe initially relied on voluntary measures until the accelerated virus spread forced stricter measures, but only belatedly. In the UK, Prime Minister Boris Johnson tried to portray inadequate preparedness as a foresighted strategy: “We can turn the tide within the next 12 weeks.”
At first, Johnson, who eventually contracted the virus himself, advocated “herd immunity” as a new strategy, relying on the advice of a group of epidemiologists. The idea was to keep virus transmission at low levels until a vaccine was available. A long lockdown was deemed impractical, due to the negative economic impact.
One report from Oxford University even claimed that the UK had already achieved herd immunity. It presumed that more than half of the population had had the virus and recovered. So, there was no longer any need to trace the contacts of every suspected case. UK would only test people who were admitted to hospitals.
To avoid a second peak in the winter, Sir Patrick Vallance, the U.K.’s chief scientific adviser, said the UK would suppress the virus “but not get rid of it completely.” While it could protect vulnerable groups, such as the elderly, herd immunity would reduce transmission in the event of a winter resurgence. In effect, Vallance thought “60 percent” of people would need to be infected for herd immunity.
In reality, herd immunity is neither a new idea nor a strategy. The idea first evolved in the 1920s. It was recognized as a recurring phenomenon when, after a significant number of children had become immune to measles, new infections temporarily decreased. As a result, mass vaccination to induce herd immunity became common.
However, as of yet, there’s no vaccination against COVID-19. And access to adequate, available and safe vaccination or therapies may take until spring 2021, or longer. Moreover, no country should ever rely on a highly contagious and deadly infectious agent to create an immune population.
Without effective vaccine, risk groups – the elderly, those with chronic pulmonary conditions, hypertension, diabetes and asthma patients, and those without adequate access to affordable health care – would be condemned into a premature death. That’s the worst kind of eugenics in the 21st century.
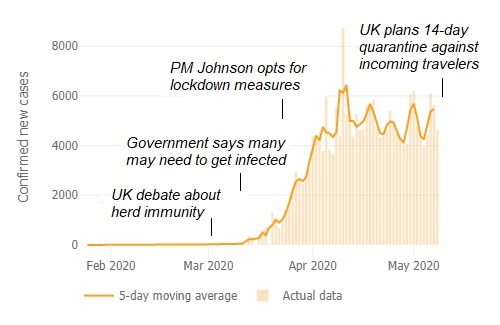
Eventually, the idea of herd immunity was rejected in the UK as unrealistic as the government finally opted for stricter lockdown measures that China, Hong Kong and South Korea had opted for already in January. Meanwhile, the epidemic curve had been fattened – not flattened – for some 6-8 weeks (Figure).
In Wuhan and Hubei, a faster infection rate had resulted in a strained healthcare system, many daily hospital visits and many infected people being turned away. That’s why social distancing was adopted to contain the spread. The goal was to “flatten the curve” quickly to reduce the potential of the virus to spread exponentially.
Despite the rejection of the idea of herd immunity, most countries in Europe and North America have in fact adopted a (failed, partial) version of it. Since they resorted to social distancing only belatedly, their health care systems became overloaded, healthcare professionals were penalized and the virus got a free ride.
Due to the belated and ineffective responses, these countries – from the U.S. to the Euro area and the UK – effectively fattened the curve before more determined efforts to flatten it. And that has broad ramifications. First, the human costs – infection cases and fatalities – will prove far higher than initially expected.
Second, in a global, interconnected economy, it is the weakest links that determine the future of the whole, through flows of trade, investment and mobility. That’s why, when countries that failed to contain the virus exit from lockdowns, they may serve as reservoirs of future infections elsewhere.
Third, the rise of imported cases in China, Hong Kong, and South Korea in the past weeks are just a prelude for waves of potential imported infections later in 2020.
Fourth, since COVID-19 is a global pandemic, it has potential to become endemic, which means elevated long-term risks in emerging and developing countries that have relatively weaker healthcare systems.
Finally, since the de facto herd immunity in the West has caused the virus to multiply into millions of effective cases, the potential for new mutations will be heightened, which will add to uncertainty while complicating the hoped-for vaccine response.
The cost of complacency
As China and other countries that mobilized early and broadly against the virus have shown, effective containment can dramatically lower the number of cases and deaths and thus drastically minimize the economic damage.
In the UK, the tragedy of the missed opportunities is particularly painful. At the time of the herd immunity debate in mid-March, when Chinese and South Korean measures were still shunned as too “authoritarian” and “invasive,” there were some 1,400 recorded cases and 50 deaths in the UK. As in the US, inadequate testing virtually ensured that thousands more were not detected, while the opportunity window for containment was missed.
As a result, today, less than 2 months later, the pandemic has cost the UK some 220,000 cases and 32,000 deaths. In 8 weeks, the recorded cases have multiplied almost 160-fold and deaths by 640 times, respectively. Worse, the curve hasn’t been flattened yet.
But that’s not the end of the bad news. Like other contagious network effects, what has happened in the UK (and the US and other advanced economies that responded to the pandemic challenge too late) won’t stay within its borders. When the UK and other advanced economies exit their lockdowns in the coming weeks, the costs of their failures have potential to further spread worldwide.
Even when less prosperous economies, have tried to flatten the curve with stricter and longer quarantines, they will soon have to cope with inflows of people and goods from advanced economies where containment failed, proved partial and resulted in defectiveherd immunity.
The kind of imported infections that China, Hong Kong, South Korea and other relatively successful virus fighters have recently witnessed could then become a new norm around the world.
The time to prepare for these imported infections is now.
The commentary is based on Dr Steinbock’s briefing on May 9 and report The Tragedy of Missed Opportunities: The COVID-19 Human Costs and Economic Damage (SIIS)

