Why Neural Stem Cells May Be Vulnerable To Zika Infection
Zika’s hypothesized attraction to human neural stem cells may come from its ability to hijack a protein found on the surface of these cells, using it as an entryway to infection. In Cell Stem Cell on March 30, researchers at the University of California, San Francisco show that the AXL surface receptor, normally involved in cell division, is highly abundant on the surface of neural stem cells, but not on neurons in the developing brain.
The neural stem cells that express AXL are only present during the second trimester of pregnancy. These cells, called radial glial cells, give rise to the variety of cell types (e.g., neurons and astrocytes) that help build the cerebral cortex. The researchers also found AXL expressed by the stem cells of the retina. Disruption of this range of cell types is consistent with the multiple symptoms associated with Zika infection in the developing fetus–including microcephaly, a brain lacking in folds, and eye lesions.
“While by no means a full explanation, we believe that the expression of AXL by these cell types is an important clue for how the Zika virus is able to produce such devastating cases of microcephaly, and it fits very nicely with the evidence that’s available,” said senior study author Arnold Kriegstein, director of the Eli and Edythe Broad Center of Regeneration Medicine and Stem Cell Research. “AXL isn’t the only receptor that’s been linked with Zika infection, so next we need to move from ‘guilt by association’ and demonstrate that blocking this specific receptor can prevent infection.”
Kriegstein’s lab has a long-time interest in brain development. When the Zika outbreak hit, first authors Tomasz Nowakowski and Alex Pollen realized from previous studies that viruses similar to Zika–such as Dengue virus–seem to use AXL as an entry point to infection. They then used gene expression analysis (single-cell RNA sequencing) to look for AXL’s presence across different cell types in mouse brain, ferret brain, human stem cell-derived brain organoids, and developing brain tissue in humans. Each of the models showed expression of AXL by the radial glial cells.
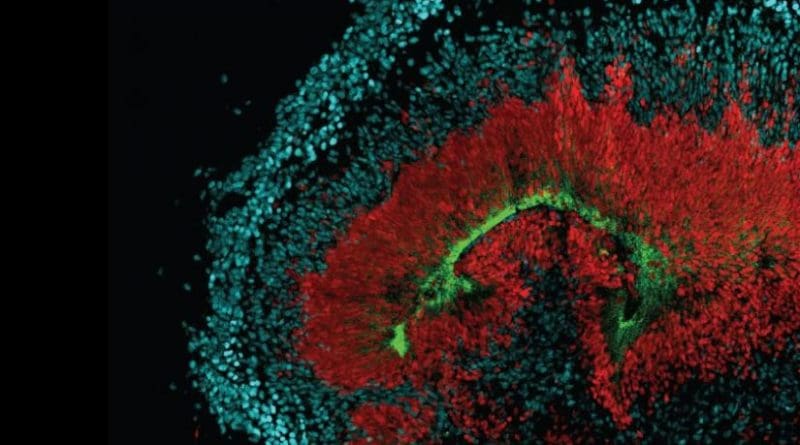
The researchers then used antibody trackers (immunohistochemistry) in the developing tissues and organoids to find out where the AXL receptor was most likely to be found on the neural stem cells. They found that AXL aggregates toward areas where the neural progenitors come into contact with either cerebrospinal fluid or blood vessels. This unique position would give a virus such as Zika an easy way to reach a vulnerable population of host cells.
“We still don’t understand why Zika in particular is so virulent to the developing brain,” Kriegstein said. “It could be that the virus travels more easily though the placental-fetal barrier or that the virus enters cells more readily than related infections.”
Pending confirmation that Zika is using AXL for neural stem cell entry, the Kriegstein group is interested in exploring if the receptor could be exploited for therapeutic purposes. Since the protein is important for neural stem cell proliferation, it is unlikely that blocking AXL will be an option in the fetal brain. But perhaps there’s a way to treat women at risk with an AXL inhibitor to stop Zika getting into the developing fetus in the first place.