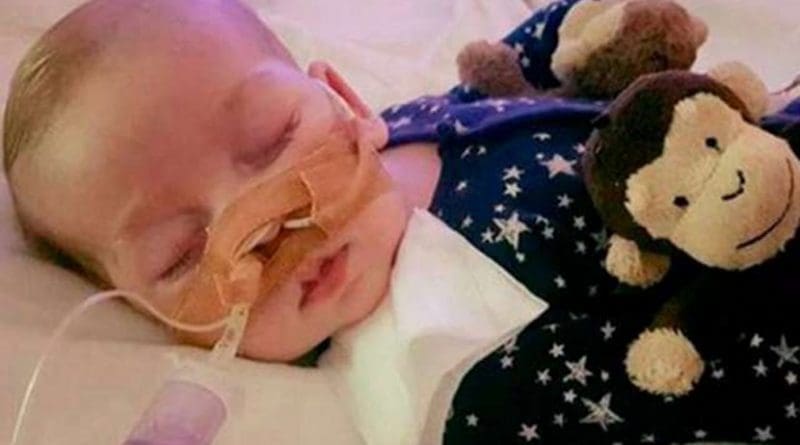
How Can We Achieve Greater Balance In Future Cases Like Charlie Gard’s
According to Professor Dominic Wilkinson at the Oxford Uehiro Centre for Practical Ethics, it is in the interests of all children that cases like Charlie Gard’s are accompanied by fair, accurate, and balanced discussion – and he asks, how can we achieve greater balance in future cases?
Difficult and ethically challenging discussions about life-prolonging treatment for a seriously ill child, usually take place privately, between parents and doctors, he explains. However, in the recent Charlie Gard case, these discussions have taken place in public, on a wide global stage.
The court of public opinion “is surely the worst possible place for ethically complex decisions,” writes Wilkinson. The intense media attention and debate about Charlie Gard led to abuse and threats to staff and to Charlie’s family. Unrealistic or unfounded claims may also have provided a false hope and contributed to the protracted legal battle.
So, how can we achieve greater balance in future, he asks?
One option would be to maintain the anonymity of any child at the heart of a dispute over treatment. While anonymity might be better for the child, he points out that it can “limit parents’ options, making it harder to fundraise for treatment and potentially harder to identify supportive expert opinion. It also conflicts with freedom of the press and raises concerns about lack of transparency in decision making.”
Another possible solution would be to allow (or require) medical professionals to make public the medical evidence on which they are basing their decisions. “That would enormously increase transparency, and help ensure that any wider discussion is based on relevant and verifiable facts. It would, however, breach the child’s confidentiality.”
Wilkinson suggests several ways forward, including gathering and publishing data on the frequency of conflicts and their outcome “to help put cases like Charlie Gard into a broader context and identify better ways to resolve them.”
Where disagreements have reached the court, he suggests making available some of evidence and arguments underpinning professionals’ decisions to allow a more realistic understanding of the basis for these decisions.
He also sounds a note of caution for the media and the wider community about relying on the opinion of professionals who have not accessed all the clinical details.
The public attention and debate around Charlie Gard hasn’t been all bad, writes Wilkinson. “It has brought wider attention to the potential futility of medical treatment, to the suffering of families of children with life-limiting illness, and to important ethical questions about the rights of sick children and the respective roles of parents and health professionals in protecting them.”
Sound ethical analysis depends on knowing more than just the scientific and medical facts, he says. “But without the facts, or with incorrect facts, there is a real danger of jumping to incorrect and potentially harmful conclusions. It is in the interests of all children that cases like Charlie Gard’s are accompanied by fair, accurate, and balanced discussion,” he concludes.