Brain Disconnections May Contribute To Parkinson’s Hallucinations
Researchers have found that disconnections of brain areas involved in attention and visual processing may contribute to visual hallucinations in individuals with Parkinson’s disease, according to a new study published online in the journal Radiology. The disconnected brain areas seen on functional MRI (fMRI) may be valuable in predicting the development of visual hallucinations in patients with Parkinson’s disease.
Hallucinations are sensations that seem real but are created in a person’s mind. A person having a hallucination may see, hear or feel something that is not actually there. According to the National Parkinson Foundation, visual hallucinations can be a complication of Parkinson’s disease.
“Visual hallucinations in Parkinson’s disease are frequent and debilitating,” said study author Dagmar H. Hepp, M.D., from the Department of Neurology and the Department of Anatomy and Neurosciences at VU University Medical Center (VUMC) in Amsterdam, the Netherlands. “Our aim was to study the mechanism underlying visual hallucinations in Parkinson’s disease, as these symptoms are currently poorly understood.”
Studies using fMRI to investigate visual hallucinations in patients with Parkinson’s disease are rare and have been mainly limited to task-based methods using activities that involve visual stimulation or cognitive tasks. However, the authors note that the presence of visual hallucinations is strongly linked to the development of cognitive decline in patients with Parkinson’s disease. Cognitive deficits may influence a patient’s ability to perform specific tasks during an fMRI exam.
For this study, researchers used resting-state fMRI to examine the connectivity, or communication, between brain areas. Resting-state fMRI is a method of brain imaging that can be used to evaluate patients not performing an explicit task. The connectivity was measured in 15 patients with visual hallucinations, 40 patients without visual hallucinations, and 15 healthy controls by calculating the level of synchronization between activation patterns of different brain areas.
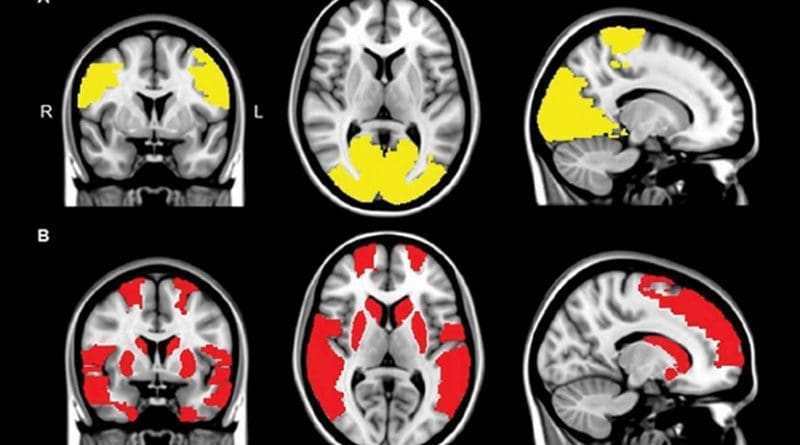
The results showed that in all the patients with Parkinson’s disease, multiple brain areas communicated less with the rest of the brain as compared to the control group. However, in patients suffering from visual hallucinations, several additional brain areas showed this decreased connectivity with the rest of the brain, especially those important in maintaining attention and processing of visual information.
“We found that the areas in the brain involved in attention and visual processing were less connected to the rest of the brain,” said study author Menno M. Schoonheim, Ph.D., from the Department of Anatomy and Neurosciences at VUMC. “This suggests that disconnection of these brain areas may contribute to the generation of visual hallucinations in patients with Parkinson’s disease.”
While there are no direct therapeutic implications for patient care based on the research, the authors note that future studies could indicate whether techniques that could stimulate the areas with decreased connectivity could be helpful to treat visual hallucinations in people with Parkinson’s disease.