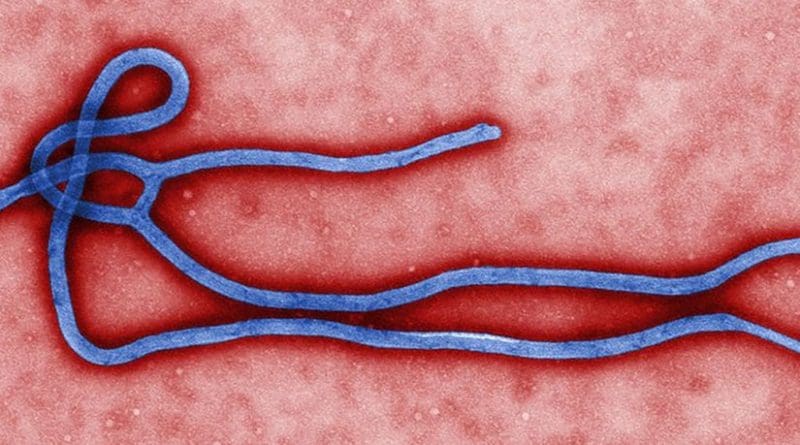
Ebola Virus Genome Provides Clues To Repeated Disease ‘Flare-Ups’ In Western Africa
Ebola virus samples taken from patients in Liberia in June 2015 are strikingly similar in their genetic makeup to other Ebola virus sequences from Western Africa, according to research published online today in the journal Science Advances. The study sheds light on several aspects of the “flare-ups” that have occurred in Liberia since the country was initially declared free of Ebola virus disease.
As described in the paper, genomic analysis and the epidemiological investigation indicate that the June 2015 flare-up was a re-emergence of a Liberian transmission chain originating from a persistently infected source. This was also the case with a March 2015 Liberian flare-up. Neither event was caused by re-introduction of the virus from an animal reservoir or from a neighboring country with active person-to-person transmission, according to the research team. While the March flare-up was traced to sexual contact, no definitive link has been found for the June event.
“When the June cluster of cases was first detected, the initial expectation of investigators was that it likely originated from a re-introduction of the virus from Sierra Leone or Guinea, where human-to-human transmission was active,” explained study co-first author Jason T. Ladner, Ph.D., of the U.S. Army Medical Research Institute of Infectious Diseases (USAMRIID). “This explanation was favored because the typical route of Ebola virus transmission is through infectious body fluids from individuals in the acute phase of the disease, when they are most symptomatic.”
However, genomic sequencing, combined with epidemiological investigation, indicated that the cases did not represent a re-introduction from a neighboring country, but instead were the result of virus transmission from a “persistently infected” source within Liberia–meaning, for example, a disease survivor who continued to carry the virus for several months.
“Although this finding did not necessarily play a major role in the control of this particular cluster, it certainly emphasized the risk for additional flare-ups, even within areas where active spread of the virus has been stopped,” Ladner said. “This understanding has led to heightened vigilance, which has allowed for rapid response to the additional flare-ups that have occurred.”
Ebola virus causes severe hemorrhagic fever in humans and nonhuman primates with high mortality rates and continues to emerge in new geographic locations, including Western Africa, the site of the largest recorded outbreak to date. More than 28,000 confirmed, probable and suspected cases have been reported in Guinea, Liberia and Sierra Leone, with more than 11,000 reported deaths, according to the World Health Organization.
In the paper, the research team–which includes scientists from the U.S. Centers for Disease Control and Prevention, the Liberian Ministry of Health, and USAMRIID–points out the risk of Ebola virus disease flare-ups even after an outbreak is declared to be over. Since the June 2015 flare-up, at least four more documented flare-ups have occurred (2 in Liberia, 1 in Sierra Leone and 1 in Guinea), according to the authors.
“From an epidemiological standpoint, this research demonstrated the value of full genome sequencing during an outbreak,” said co-senior author Gustavo Palacios, Ph.D., of USAMRIID. “The viral genomes from the June flare-up were compared to what had been sequenced already, which allowed us to determine that the virus was indeed Liberian in origin. This helped confirm what the epidemiological teams were finding in their investigation and focused efforts on looking for potential sources of persistent infection within and around the affected community.”
According to Palacios, the study was made possible by the in-country laboratory capability established by USAMRIID in 2015 in collaboration with the Liberian Institute for Biomedical Research (LIBR) and the Liberian Ministry of Health. This state-of-the-art, high-throughput sequencing facility allows the team to conduct near real-time genomic sequencing.
The viral genomes also helped to tell another story, said USAMRIID co-first author Michael R. Wiley, Ph.D. He noted that a reduced rate of evolution was associated with the June 2015 flare-up–meaning that the genetic signature of the virus had not changed significantly over time. When the team looked at the March 2015 cluster, which had been associated with sexual transmission, they found the same signature–a reduced rate of evolution.
That “signature” could be a useful tool for evaluating the source of future outbreaks, according to Wiley. Specifically, it indicates that the virus likely replicates at a lower rate during persistent infections, as compared to the acute phase of the disease.
“It’s not clear what processes are driving this reduction in replication rate, or what role this change in rate may play in establishing or maintaining persistent infections,” Wiley said. “It’s important, therefore, to better understand the nature of these persistent infections in order to prevent the continuation of an outbreak once human-to-human transmission via acute individuals is controlled. Also, there is a need to develop treatment methods that are effective at curing these persistent infections, which may be contributing to the long-term chronic health problems associated with some Ebola virus disease survivors.”
Palacios said the team is continuing to investigate additional Ebola virus flare-ups that have occurred in Liberia, including the cluster of cases in November 2015 and the recent cluster of cases that occurred earlier this month. They are also further investigating the rate of viral evolution during persistent infections by sequencing Ebola virus genomes from the semen of disease survivors.